
Leg pain and swelling are common complaints that can stem from something as simple as prolonged sitting or as serious as a blood clot. A vein specialist provides focused evaluation and treatment to determine whether veins are the source of symptoms and to reduce long-term risks to mobility and skin health. Clinics such as Metro Vein offer expertise in accurate diagnosis, minimally invasive treatment options, and personalized care plans for lasting results. This article explains when to see a vein specialist, the common vein-related causes of leg pain and swelling, how specialists diagnose issues, available treatment options, what to expect at an appointment, and practical steps to support long-term vein health—designed for busy professionals who need clear, actionable guidance to get back to work and daily life with confidence.
When to See a Vein Specialist
Leg pain and swelling don’t always mean a vein problem, but there are specific signs that make specialist evaluation important. A vein specialist (phlebologist, vascular surgeon, or interventional radiologist who focuses on venous disease) should be consulted when any of the following occur:
- Persistent swelling in one or both legs that doesn’t improve with rest or elevation.
- Visible bulging, twisted veins (varicose veins) associated with aching, heaviness, or cramping.
- New redness, warmth, or intense pain in a leg, these can signal a blood clot (deep vein thrombosis, DVT) and require urgent attention.
- Skin changes over the lower leg or ankle, such as darkening, thickening, or ulcers that won’t heal.
- Recurrent leg fatigue or discomfort that interferes with work, exercise, or sleep.
Early evaluation matters. Left untreated, chronic venous problems can progress to skin breakdown, recurrent infections, or impaired mobility. For professionals with tight schedules, entrepreneurs, agency leads, and site owners, recognizing these triggers and booking a focused consult can prevent longer interruptions to productivity.
Common Causes of Leg Pain and Swelling Related to Veins
Vein-related leg symptoms stem from distinct conditions with different risks and treatments. A brief look at the most common culprits helps frame expectations before a specialist visit.
Varicose Veins and Spider Veins
Varicose veins are enlarged, tortuous surface veins caused by weakened vein walls and valve failure. They commonly produce aching, heaviness, nighttime cramps, and visible rope-like veins. Spider veins are smaller, branching venules that mainly cause cosmetic concerns but can coexist with deeper venous disease. While not typically life-threatening, varicose veins can significantly reduce comfort and function.
Chronic Venous Insufficiency (CVI)
CVI occurs when venous valves fail to return blood efficiently to the heart, causing pooling and increased pressure in the lower legs. Symptoms include swelling (especially after prolonged standing), skin discoloration, itching, and, in advanced cases, venous ulcers. CVI is progressive without treatment and is often the underlying condition behind recurrent swelling and skin problems.
Deep Vein Thrombosis (DVT) and Post‑Thrombotic Syndrome
DVT is a blood clot in a deep vein, usually in the calf or thigh. It commonly causes sudden unilateral swelling, pain, and warmth. DVT is a medical emergency because clots can travel to the lungs (pulmonary embolism). After DVT, some people develop post-thrombotic syndrome, chronic pain, swelling, and skin changes caused by venous obstruction and valve damage.
Lymphedema and Nonvenous Causes to Consider
Not all leg swelling stems from veins. Lymphedema (lymphatic system dysfunction), heart failure, kidney or liver disease, medication side effects, and localized infection can cause swelling. A vein specialist will often collaborate with primary care, cardiology, or vascular medicine to rule out or manage nonvenous contributors.
How Vein Specialists Diagnose Vein Problems
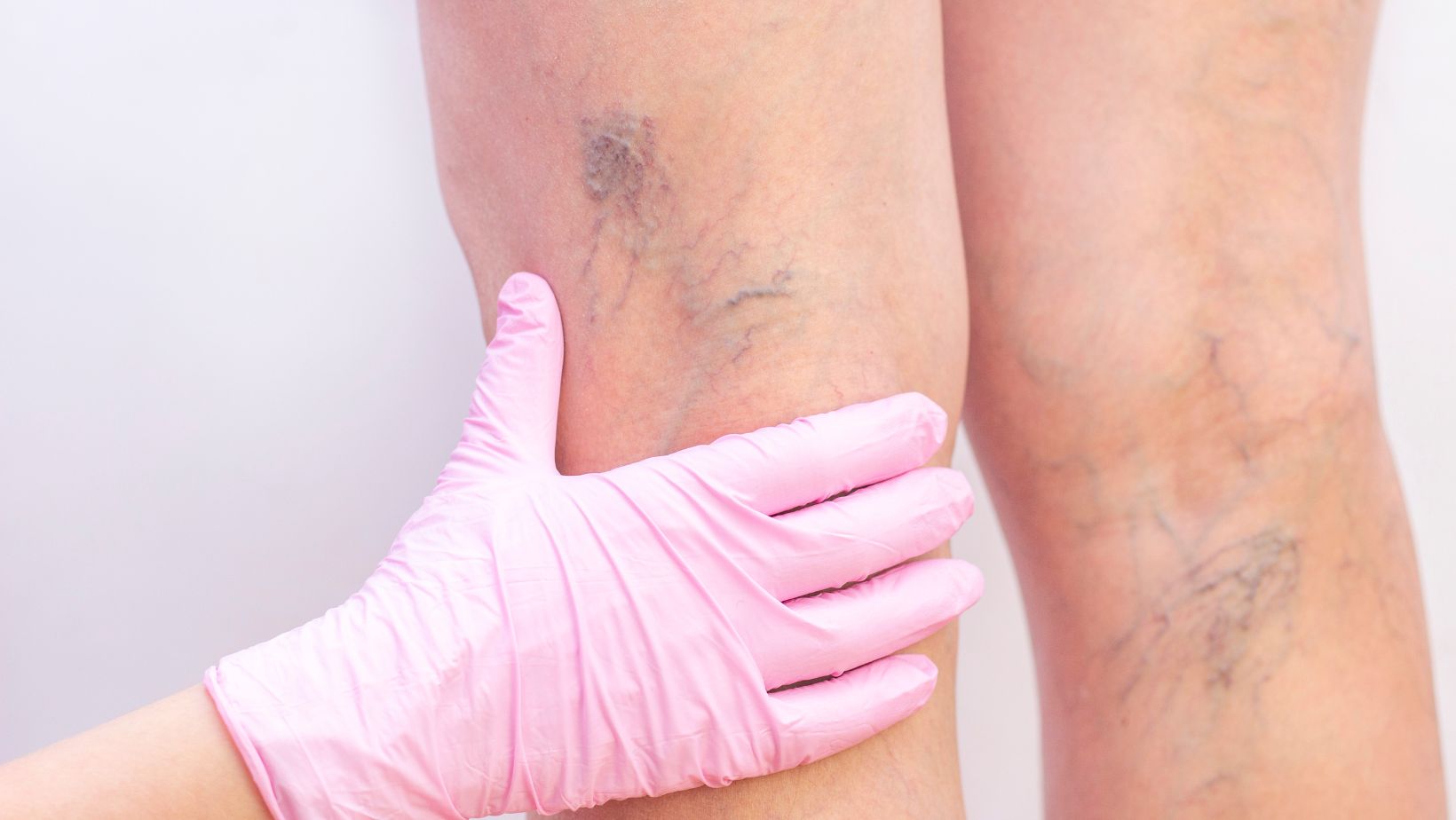
Accurate diagnosis relies on a combination of careful history, targeted physical exam, and imaging.
Medical History and Physical Examination
The specialist collects a focused history: symptom onset and pattern, prior blood clots, family history of venous disease, recent immobility or travel, and medications (like hormone therapy or blood thinners). The clinician inspects the legs while the patient is standing to assess varicose veins, swelling distribution, skin changes, and any ulcers. This step helps prioritize tests and tailor treatment.
Venography, Blood Tests, and Additional Evaluations
If DVT is suspected, blood tests like D‑dimer can be supportive, although imaging is essential. Venography is less common but useful for detailed vascular mapping. Specialists may also evaluate for coagulation disorders when clotting risk is unexplained or coordinate cardiovascular evaluation if systemic causes are suspected.
Treatment Options Offered by Vein Specialists
Treatment ranges from conservative care to minimally invasive procedures and, rarely, open surgery. The specialist recommends options based on cause, symptom severity, and patient goals.
Conservative and Medical Therapies (Compression, Medications, Lifestyle)
Compression stockings remain a first-line therapy for symptomatic varicose veins and mild CVI. They reduce swelling and improve comfort. Specialists may also prescribe anti-inflammatory medication, short courses of anticoagulation for acute clots, or venotonic agents in select cases. Lifestyle measures, weight management, leg elevation, and avoiding prolonged standing complement medical care.
Minimally Invasive Procedures (Sclerotherapy, Endovenous Ablation, VenaSeal)
- Sclerotherapy: Injection of a sclerosant into small-to-medium veins to collapse them, effective for spider veins and some varicosities.
- Endovenous thermal ablation (radiofrequency or laser): A catheter heats and closes the diseased vein; recovery is quick, and outcomes are durable.
- VenaSeal (medical adhesive): A cyanoacrylate glue that seals the vein without thermal energy: useful for patients who prefer to avoid tumescent anesthesia.
These procedures are typically outpatient, performed under local anesthesia with rapid return to activity.
Managing Acute Conditions Like DVT
For DVT, early anticoagulation is crucial to prevent clot extension and pulmonary embolism. Some patients may need thrombolysis (clot-dissolving therapy) or mechanical thrombectomy when clots are extensive and limb-threatening. After DVT, long-term strategies include compression, possible endovascular intervention for chronic obstruction, and anticoagulation plans tailored to the clot cause and risk.
Preparing for Your Appointment and What to Expect
A little preparation makes the visit more efficient and ensures the specialist has what they need to make treatment recommendations.
Questions to Ask the Vein Specialist
Patients should consider asking:
- What’s likely causing my leg pain or swelling?
- Do I need imaging today? If so, which test?
- What are the treatment options and their recovery times?
- What are the risks and expected benefits of each option?
- Will treatment allow me to return to work and exercise, and when?
- Are there measures to reduce recurrence?
These targeted questions help busy professionals get concise, actionable answers during limited appointment time.
How to Prepare: Tests, Clothing, and Insurance/Referral Tips
Wear loose shorts or clothing that gives easy access to the lower leg. Bring a list of current medications and prior imaging or surgical records. Check with the insurer about coverage for diagnostic ultrasound and interventions: many plans require prior authorization. If a referral is needed, arrange it ahead of time to avoid delays.
Follow‑Up Care and Recovery Expectations
Most minimally invasive procedures allow same‑day discharge and quick resumption of daily activities. Compression stockings are often recommended for a short period post-procedure. Specialists schedule a follow-up duplex ultrasound to confirm vein closure and to monitor healing. Recovery expectations depend on the treatment chosen: clear aftercare instructions and a follow-up plan improve outcomes.
Preventing Recurrence and Supporting Long‑Term Vein Health
After successful treatment or when managing chronic venous disease conservatively, adopting consistent habits reduces recurrence and supports leg comfort.
Daily Habits: Movement, Weight Management, and Leg Elevation
Regular movement, brief walks every hour, calf raises, and avoiding prolonged standing promote venous return. Maintaining a healthy weight reduces venous pressure and symptom burden. Elevating the legs above heart level for 15–20 minutes several times a day helps drain pooled fluid.
Compression Stockings, Exercise, and Skin Care Strategies
Compression stockings remain a cornerstone for many patients, especially those with CVI or after DVT. Graduated compression improves comfort during long days at a desk or on flights. Low-impact exercises, walking, cycling, and swimming, strengthen calf muscles that act as a natural pump. For those with skin changes, gentle moisturizing, prompt treatment of infections, and avoiding trauma to the lower legs prevent complications.
When to Return for Care and Red Flags to Watch For
Follow up with the specialist if symptoms recur or worsen. Seek immediate care for sudden unilateral swelling, chest pain, or shortness of breath, signs that require emergency evaluation. Early re-assessment preserves limb health and reduces the chance of chronic complications.
Conclusion
Vein specialists offer targeted evaluation and a range of effective treatments for leg pain and swelling related to venous disease. For professionals juggling demanding schedules, early identification and treatment can prevent prolonged downtime and progressive complications. A single focused visit, armed with a brief symptom history, prior records, and key questions, often clarifies the cause and maps a practical plan. Maintaining movement, using compression when indicated, and following specialist guidance supports long-term vein health and lets people return to work and life with greater confidence and comfort.







